How does hep C affect the liver?
The liver is the second largest organ in the body and carries out many functions to help keep you healthy. The liver’s main function is to clean your blood of toxins by producing bile to break down fat into energy. In hep C, liver scarring (fibrosis) can prevent the liver from doing its job.
If you have hepatitis C, it can damage your liver. In some cases, after more than 20 years, hepatitis C can lead to cirrhosis (severe scarring), liver failure and sometimes liver cancer.
That’s why it is important to get tested if you can say ‘yes’ to any of the hepatitis C risk factors or symptoms.
Hepatitis C


– is caused by the hep C virus (HCV)


– spreads when the blood from a person infected with the hepatitis C virus enters the body of someone who is not infected


– begins as an acute infection (lasting less than 6 months)


– becomes chronic (long-lasting) in more than half of people who become infected


– often doesn’t present any symptoms, but can lead to serious health complications


– can be cured.
Cure means the hep C virus is not detectable in your blood 3 months after treatment has ended.
The potential progression of hep C following exposure to the virus
ACUTE hep C infection




What can happen if hepatitis C is left untreated?
Having hep C doesn’t automatically mean you’ll experience symptoms or develop liver disease. But the longer you live with it, the more likely you will have some sort of liver damage.
When the liver becomes damaged, it forms scar tissue. When the liver first becomes scarred, it is known as fibrosis. When the scarring increases so much that the liver can’t function properly, this is known as cirrhosis.
Of people with untreated chronic hep C, approximately 1 out of 5 will develop cirrhosis within 20 to 30 years.
Untreated hep C can lead to liver disease, liver failure and an increased risk of liver cancer in some people.
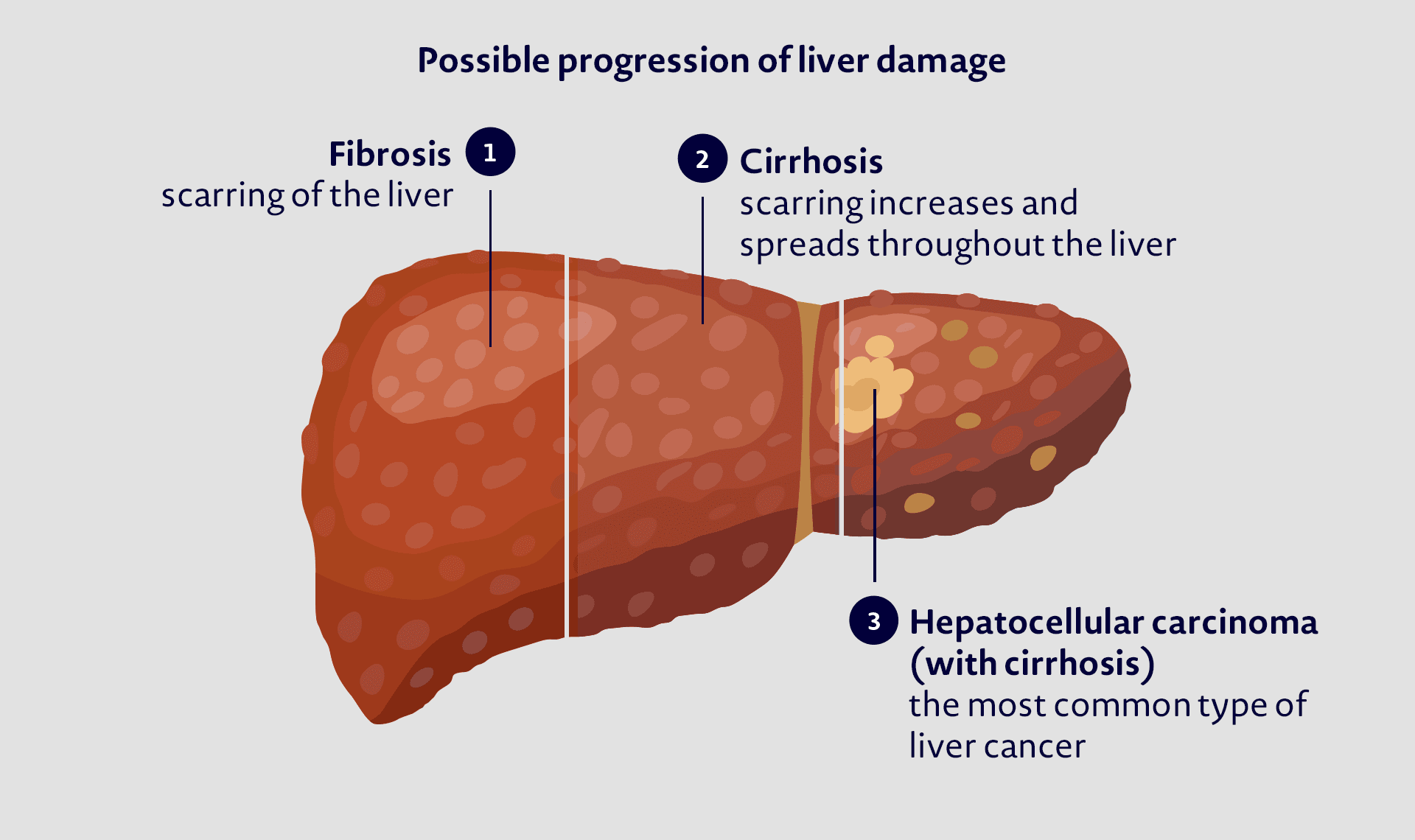
Successful treatment of hepatitis C infection can reduce the risk of developing liver failure and liver cancer.
Why it’s so important to get tested
The hep C virus is contagious and can exist in amounts of blood that are too small to see. It is spread when infected blood enters your bloodstream and can exist in traces of blood outside the body for several days to weeks.
No matter the stage of hep C infection, symptoms may not appear even though liver damage could be happening. This is why it is important to get tested.
You can check if you have any risk factors or symptoms of hep C. And if you have any questions or want to get tested, see your healthcare professional.
MORE ABOUT TESTING AND TREATMENT FOR HEP C
Early diagnosis and treatment can save lives.
Hepatitis C is one of several types of viral hepatitis
Other common hepatitis viruses include hep A and hep B. Although each virus can cause similar symptoms, they are spread in different ways and can affect the liver differently.
Hep A is transmitted by contact with faeces of an infected person. It is mainly spread by consumption of contaminated water or food.
Hep B is spread when blood or other body fluids (such as vaginal fluids or semen) from a person infected with the virus enters the body of someone who is not infected. It can be spread from mother to child during childbirth, having unprotected sex, and sharing needles and syringes or other drug-injection equipment.
Hep C is spread when your blood comes into contact with even a small amount of infected blood.
The New Zealand Hepatitis Foundation has more information on the different types of viral hepatitis.
You can be vaccinated against hep A and hep B but there is NO vaccination for hep C.